Introduction Varicose Veins
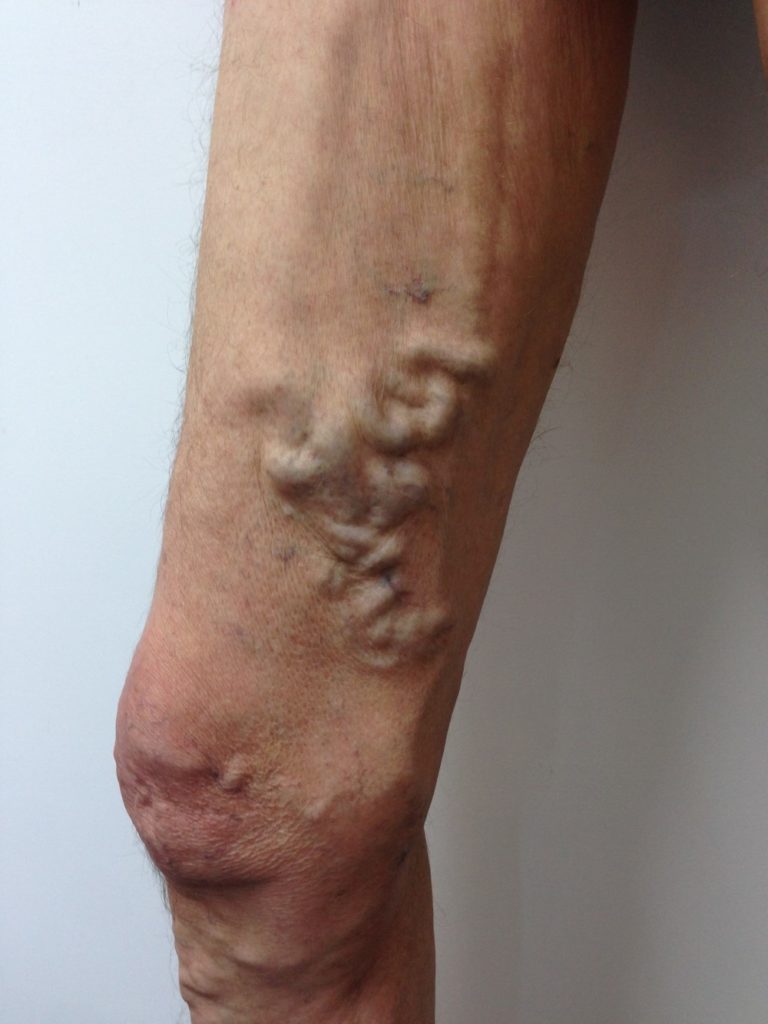
Varicose Veins 1. Varicose veins are twisted, enlarged veins. Any vein that is close to the skin’s surface (superficial) can become varicose. Varicose veins most commonly affect the veins in the legs. That’s because standing and walking increase the pressure in the veins of the lower body.
For many people, varicose veins and spider veins — a common, mild variation of varicose veins — are simply a cosmetic concern. For other people, varicose veins can cause aching pain and discomfort. Sometimes varicose veins lead to more-serious problems. Also, treatment might involve self-care measures or procedures by a healthcare provider to close or remove veins.
Symptoms of Varicose Veins
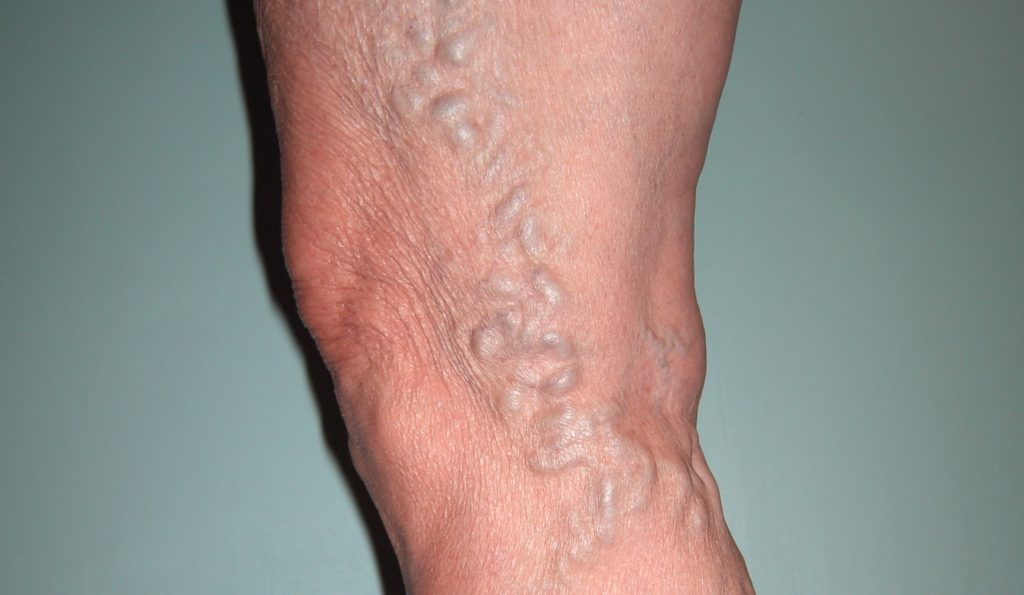
Varicose Veins 1. Varicose Veins might not cause pain. Signs of varicose veins include:
- Veins that are dark purple or blue
- Veins that appear twisted and bulging, often appearing like cords on the legs
When painful signs and symptoms of varicose veins occur, they might include:
- An achy or heavy feeling in the legs
- Burning, throbbing, muscle cramping and swelling in the lower legs
- Worsened pain after sitting or standing for a long time
- Itching around one or more of the veins
- Changes in skin colour around a varicose vein
Spider veins are similar to varicose veins, but they’re smaller. Also, spider veins are often red or blue and are found closer to the skin’s surface. In addition, spider veins occur on the legs but can also be found on the face. In addition, they vary in size and often look like a spider’s web.
Risk Factors

Varicose Veins 1. The following can increase the risk of developing varicose veins:
- Age. Ageing causes wear and tear on the valves in the veins that help control blood flow. Eventually, that wear causes the valves to allow blood to flow back into the veins, where it collects.
- Sex. Women are more likely to develop the condition. So then, hormonal changes before a menstrual period, during pregnancy, or menopause might be a factor because female hormones tend to relax vein walls. Hormone treatments, such as birth control pills, might increase the risk of varicose veins.
- Pregnancy. During pregnancy, the blood volume in the body increases. This change supports the growing baby but can also enlarge the veins in the legs.
- Family history. If other family members had varicose veins, there’s a greater chance you will too.
- Obesity. Being overweight puts added pressure on veins. (take note)
- Standing or sitting for long periods of time. Movement helps blood flow.
Complications
Complications of varicose veins, although rare, can include:
- Ulcers. Painful ulcers can form on the skin near varicose veins, particularly near the ankles. A discoloured spot on the skin usually begins before ulcer forms. See your healthcare provider immediately if you’ve developed a leg ulcer.
- Blood clots. Occasionally, veins deep within the legs become enlarged and might cause leg pain and swelling. Seek medical attention for persistent leg pain or swelling because it can signify a blood clot.
- Bleeding. Occasionally, veins close to the skin burst. Although this usually causes only minor bleeding, it requires medical attention.
Prevention
Varicose Veins 1. Improving blood flow and muscle tone might reduce the risk of developing veins that are varicose. The same measures that treat the discomfort from these veins can help prevent them. Try the following:
- Avoiding high heels and tight hosiery
- Changing your sitting or standing position regularly
- Eating a high-fibre, low-salt diet.
- Exercising
- Raising your legs when sitting or lying down
- Watching your weight
- Many doctors recommend compression socks to prevent the condition from getting worse.
Medical Treatments

Varicose Veins 1. Some medical treatments are also available to help tackle problem veins. A doctor may prescribe the following:
- Endothermal ablation. This is a procedure where heat is used to seal the affected veins.
- Ambulatory phlebectomy. This is where a doctor will puncture the skin and remove these veins through tiny slits. Scarring is usually minimal afterwards.
- Sclerotherapy. This procedure uses a particular foam to close the veins and shrink them.
- Ligation and stripping. In this procedure, the veins are surgically removed.
- Laser surgeries. Here, intense bursts of light are directed onto the vein, making it gradually fade and disappear.
- Endoscopic vein surgery. During this surgery, a tiny video camera is inserted into the leg to help the surgeon see better. Removal of the veins then takes place via a series of small incisions.
Sclerotherapy
Sclerotherapy effectively treats varicose and spider veins. It’s often considered the treatment of choice for small varicose veins.
Sclerotherapy involves injecting a solution directly into the vein. The sclerotherapy solution causes the vein to scar, forcing blood to reroute through healthier veins. Hence, the collapsed vein is reabsorbed into local tissue and eventually fades.
After sclerotherapy, treated veins tend to fade within a few weeks, although occasionally it may take a month or more to see the full results. So then, several sclerotherapy treatments may be needed in some instances.
In Conclusion
As we age combined with our lifestyle or family history means we can suffer from varicose veins. They are hated by those who get them but are treatable by a number of procedures. The important thing to remember is once you notice them seek medical advice. Because your doctor can recommend the best treatment for what you have.
Important Note *
Remember that everyone is different, and it is ultimately YOUR RESPONSIBILITY to find what your body responds to. So please do your due diligence before trying anything new, including getting Medical Advice to ensure your safety and peace of mind.
Connect with me and leave a comment or two on my social media.


2 replies on “Varicose Veins 1”
Thanks a lot for the this exercise about varicose veins. Now we have an idea for control and care.
Sarah
Hi Sarah, thank you for your kind words, I hope you have a very merry Christmas, all the best Ian